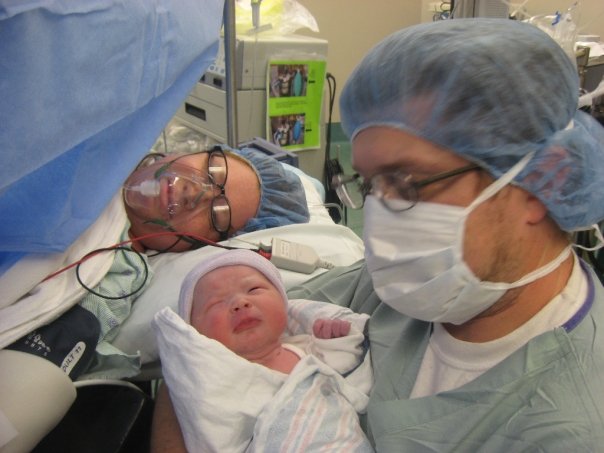
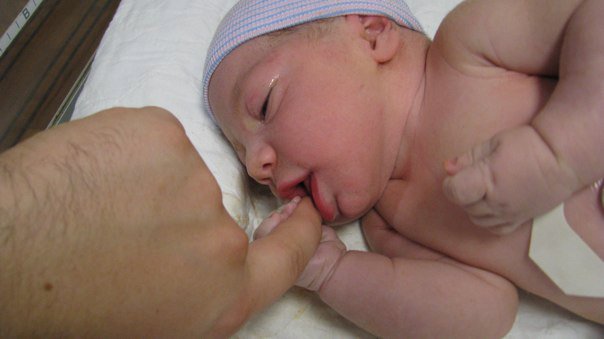
July is birth story month at the Motherhood Collective. Reading the good, the bad, the ugly and the BEAUTIFUL experiences of other mothers gives us a real appreciation for the strength we have in childbirth. Hopefully these stories will inspire you.
Today's post is written by Kerissa Scott, a regular attendee at the Motherhood Cafe. Knowing her birth story, we asked her to share it and she graciously agreed. Part One of her story was posted on Monday and ended with the birth of her son. Part Two of her story deals with the time afterward in the NICU.
My Introduction to the NICU
I have always had a passion for preemie babies. It was my absolute favorite clinical in nursing school and I dreamed of becoming a NICU nurse before I found out I was pregnant. So I had been around very, very small babies with many serious issues. However, no amount of time spent there could have prepared me for my own child being the patient.
My dad had been able to go with the baby to the NICU, and I believe my mom went to see him before I did as well. Thinking back, I may have “sent” them to watch over him. I had to wait until the epidural fully left my body and I could walk. I think this took about 30 minutes.
My son was on a ventilator, which was breathing for him, and there was tape all across his face to hold it in place. He had several wires coming out of his belly button - if they are able to, the hospital uses the umbilical arteries in preemies rather than having to stick them for an IV. There were “leads” on his chest, measuring his respirations, and a pulsometer on his wrist. There are so many machines, making all sorts of different noises, and each baby has several machines, so there was a ton of beeping, whooshing, and all sorts of other noises. He was in an incubator, but luckily for this first visit, it had an open top, so i was able to see him easily, touch him, and love on him. I wasn’t able to stay very long, because I was also still a patient and they wanted to monitor me.
The next time I came in, they had put him under contact precautions due to my MRSA. I still had not been able to get my 3 nasal swabs cleared, which automatically put him at risk. It was all so much overkill, but standard procedure. This killed me, because it meant I could not touch him without gloves on. I argued and argued about how I had already touched him and how if he had it, it was from me, so it shouldn’t matter. Every valid argument I could come up with, I threw at them. But alas, I had to wait for the nasal swabs. I remember I would pull off the tip of the glove on one finger, just so I could get that skin to skin touch that newborns and mamas so desperately need.
 The next day he was taken off the ventilator and put on a CPAP machine, one step up! The nurses measured his blood gas levels several times a day, which determined any changes in his respiratory therapy. His bilirubin levels went up (translation: he had jaundice) and he was put under the glorious blue lights with the cutest little shades for his eyes. He was also receiving TPN via IV (total parenteral nutrition), basically food in liquid form, since they had not started feeding him yet.
The next day he was taken off the ventilator and put on a CPAP machine, one step up! The nurses measured his blood gas levels several times a day, which determined any changes in his respiratory therapy. His bilirubin levels went up (translation: he had jaundice) and he was put under the glorious blue lights with the cutest little shades for his eyes. He was also receiving TPN via IV (total parenteral nutrition), basically food in liquid form, since they had not started feeding him yet.
I would go back and forth from my room to the NICU all day. Pumping every 3 hours, possibly getting in a phone call, and then straight to his side. I’m not sure which day it was but I know one day I stayed so long that I started bleeding down my leg - my pad had totally filled up and was leaking all over, creating a puddle beneath me. It was pretty embarrassing because in Virginia Baptist, there are no curtains or anything separating the babies, so everyone else who was in there visiting their newborns saw me. My nurse was called and had to come get me in a wheelchair.
Everyone always asked me how I picked my son’s name. I was discharged 2 days after he was born, but was able to stay in my room as “hospitality”, so I could be close and not have to drive back and forth (especially because I was pumping and technically couldn’t drive for 14 days). However, they told me they could not officially discharge me without giving him a name, so I was given I think like an hour deadline to have a name. The nurses and everyone asked all the time what his name was, but I really didn’t feel like I was ready to name him. I didn’t know him well enough and hadn’t spent enough time with him. But alas, I sat down with my list next to him and went through my top picks. None of them fit. So I went back to my long list, and for some reason Levi just stood out. I always wanted an Irish name (which Levi is not), but I just knew that he was a “Levi”. So I saved the Irish part for his middle name “Reece” which means “ardent, fiery”. He had already made a name for himself in the NICU as being quite the little firecracker, pulling out all his tubes and IVs several times. He was a fighter from the beginning. Levi Reece. As soon as I said the two together, that was his name.
Settling In to Life in the NICU
At this point all of the days kind of blend together. I have notes written down with his stats for the day but a lot of it doesn’t make sense to me now. The single best description I know of regarding life with a baby in the NICU is a rollercoaster. Things can be going awesome one day, and the next your baby’s life could be in danger. Thankfully, Levi never had any life threatening issues, but there were definitely some low “lows”.
He eventually graduated from the CPAP machine to a nasal cannula, and then would be taken off the nasal cannula, only to be put back on it a few hours later. He was off it for over 5 days at one point, and then they randomly decided he needed it again. I would be told I could hold him, only to find out his levels came back too low, and they didn’t want to risk it. I finally got to hold him June 25, when he was 4 days old. We were still on contact precautions, so I had to wear a gown and gloves, but I was able to hold my baby. He would gain 30-40 grams one day (yes, I said grams, and you better believe I did a huge happy dance if he gained even 10 measly grams), and then the next day lose 50. (For some perspective: he was 1960 grams when he was born - 4 lbs 5 oz; when he was 5 days old he was 1920 grams.) When they started feeding him, his first “meal” was 4 cc of breastmilk. You can barely even measure that. But he could only “eat” if his respirations were below 70. For some reason, Levi has always been a fast breather, so a lot of our “lows” were him breathing too fast and not being able to eat. I knew that in order to come home, he needed to gain weight, which meant he needed to eat, so if he couldn’t eat, he wasn’t coming home.
His respirations caused the most controversy between the nurses and me. From nursing school, I knew that you were supposed to count for a full minute for any newborn (especially a preemie) because their breathing is so erratic. Yet many of the nurses would only could for 30, then double the number, and his respirations would be “too high” to eat or be held, etc. I began demanding they count for 60 seconds, AND let me count with them. I also knew that high respirations was not a good reason to not let me hold him. Science has proven that skin to skin contact is extremely beneficial for babies, and can calm a restless baby in seconds. So I pushed as much as I could, every time, with every nurse, to hold him; some would give in, some were cutthroat you-know-whats.
So many things have to happen in order for a baby to be ready to come home from the NICU. Most have to be able to breathe on their own, be able to drink from a bottle, and be “weaned” off the incubator to room temperature air. One day they could be doing all of these things like a champ, and the next they could not be doing any. I know I talked about this earlier, but it REALLY is a rollercoaster. And some days I felt like he would never come home. It was so hard not to compare Levi to the other babies in there. I know all babies are different, but no matter how much textbook knowledge I had or sought out, I still measured him up to his fellow NICU babies. Since I only heard little tidbits of each baby's story, I couldn’t TRULY compare them. Everyone progresses at a different rate, but if I noticed the boy next to him was being taken out of the isolette, or sent home, I was immediately discouraged.
Problems Arise
When Levi was about 11 days old, I started paying attention to EVERYTHING much more closely. I started seeing discrepancies and things the nurses ignored. He was still on the cannula, but it was rarely in his nose because he pulled it out all the time. They would tape it on his face even more to try and keep it in, but that was making his eye swollen because it was too tight. Every nurse was different - there didn’t seem to be any consistency or “protocol” they followed. Some would offer to let me bottle feed him, some would tell me he was only allowed to be gavaged (fed through his Nasogastric tube). Some nurses let me hold him for hours. Some claimed there was a 30 minute limit. I came in one day and noticed his IV had infiltrated - meaning the fluid that was supposed to be going into his vein/artery was now just going into his tissue, and his entire arm was swollen. I am the one that noticed this and pointed it out - not the nurses. Several times I found him with a poopy diaper that he had been sitting in for a while, because it was stuck to his butt. One nurse put the wrong setting on his nasal cannula air, which wasn’t remedied until the respiratory therapist came down to give him the correct cannula for the percent of oxygen (sorry if you don’t understand the medical references). I was getting incredibly discouraged and felt more and more that I needed to be next to him 24/7, which was impossible for me to do.
When he was 13 days old, I left the hospital to return home. This was the hardest thing for me to do - and looking back potentially one of the worst decisions. I still came to see him multiple times a day, but we lived 30 minutes from the hospital. I called all the time, but the nurses were only willing to share so much, or talk to me for so long. It’s hard to describe the feeling of being away from your newborn, but imagine only “visiting” your child twice a day, rather than them basically being attached to you. It was so unnatural, unnerving. Point blank: I hated it.
Levi breastfed for the first time July 9th, which I had been pushing for from the beginning; but even then they would only allow him to nurse for 10 min prior to a scheduled feeding, and then they would feed him as if he hadn’t nursed. This means if he had residual, they would base it on how much they fed him, not accounting for the extra milk he got while nursing. And if he didn’t finish his scheduled feeding, they counted it against him. They said they did this because most of the babies don’t really get anything while nursing, but when I “let down”, milk shot everywhere, so I can guarantee you he got quite a bit if his mouth was anywhere near my nipple. This almost made me want to NOT nurse him, because I felt like on the charts, it would look like he was doing worse (not finishing feedings, having residuals) if I did. Quite frustrating.
More problems started to arise. Even though he was gaining weight and doing great with feedings, they decided to mix my breastmilk with fortified formula to help him gain more, faster. As soon as they started doing this, he started having what they call “residuals”. Each time before they feed him, they pull back with a syringe on his NG tube to see if there is anything left undigested in his belly. If there is any, they measure it, and usually feed him that much less for the given feeding time. Instead of stopping the fortification, they decreased his feeding amount, which made no sense to me. He started losing weight and spitting up more. I didn’t know at the time that I could DEMAND they only feed him breastmilk. If I had known that, I definitely would have done so. It got so bad that he stopped taking feedings from a bottle altogether, and was back on an NG tube at 4 weeks old.
Here is a little excerpt from one of my updates, written in the moment. I feel like it shares my feelings at the time so much better than I could summarize now:
He had a rough few days there. Not sure if he is out of that yet or not. But he wasn't taking a bottle, or if he did, he would only take like 10 ccs (out of his 51 cc feeding). So he was basically being gavaged 24/7. His respirations are back up again. They did an xray to make sure he hadn't developed pneumonia or anything, but that looked clear.
I was super frustrated with the nurses. I felt like they are not aware of everything going on, they didn't really look through his chart to try and catch patterns, but just assessed based on the “here and now”. One Saturday morning I was there and they were severely under staffed. There were only 2 people in the NICU pretty much the whole time I was there. Babies were just left crying. They weren't getting fed, or were getting fed way late. Monitors were going off and there was no one free to check on the baby. I did NOT want to leave him there with it like that, but I had to go to my baby shower!
Also, for his feeding that visit, the nurse wanted to gavage him because his breathing was too high. I questioned it, thinking they should at least let him try, but she was pretty firm. So I kangarooed with him while he got his tube feeding, and had to fight him the whole time. He kept wanting to nurse, and trying to pull his tube out, crying, etc. It was awful.
So when I went back that night and they wanted to do the same thing, I got pushy. It was a new nurse (new to me not to the unit) and I knew she didn't know him at all. She said it’s a policy that they don't feed them if they are breathing over 70. His respirations were at 72.... so after some bickering, she recounted him, and he was 62. I pulled out all that stops that time, wanting to make this visit worth the while because he has been having so much trouble. I got her to let me take him into the parenting room. I got to breastfeed for 10 min and then she said he could "try" the bottle. He sucked the whole thing down like a champ, after having already breastfed.
I felt like if he did THAT much better for me, they must really not be trying. I knew he will probably have done better with me no matter what, because I'm his mommy. To have that big of a difference was questionable.
Let’s take a break from the stress for a funny story:
After I fed him one night, he had a really stinky diaper. I decided to just change him on my lap since he was already out of his isolette and it was a pain to put him back in. Well, clearly I should not have made that decision, or at least decided to point his butt a different way, because I got shot! I guess he was not done pooping, because he so nicely squirted the remainder onto me (an impressive distance I must say). It went all over and down my bra, yummy chunky bright yellow. I could barely stop laughing long enough to clean it up. One of the nurses there got quite the kick out of it - sharing that she had been pooped on multiple times, once even in the mouth (YUCK!).
Major drama
Okay now that you’ve had some comic relief, prepare yourself for the worst part of my story. On Monday night, July 19th, 2010, Levi was given someone else’s breast milk. How this happened doesn’t even need to be told, because it was so careless and unacceptable. This opened up all sorts of infection control issues: What is the mom whose milk he had received had HIV or some other transmittable disease? Or (more likely), what if she was smoker, or had drugs in her system? What was even more frustrating, is I brought in a bag a milk the previous day, and every single bag has to be labeled with time, date, and his personal sticker label that they give you. I accidentally forgot to label some of my bags; so, following protocol, to ENSURE no one got the wrong milk, they threw 5 bags of my milk away. Anyone who has had to pump round the clock will understand how upsetting that was. But then, to find that because they didn’t even look at the labels or double check them, Levi ended up getting someone else’s milk anyway. By the way, I found out about this via a phone call at 1 A.M. Sleep deprived, pumping round the clock, NICU mama, and they called at 1 A.M.
When I visited him the next day, the nurse told me his respirations were 72, so he couldn’t bottle feed. Except she only counted for 15 seconds. She didn’t even do 30, I mean 15 seconds? Are you kidding me? I proceeded to give her a lecture on standard procedure for measuring an infant’s respirations and demanded she count again, for the full minute. 66. Of course. He was totally ok to bottle feed, she was just being lazy. How many times did this happen while I wasn’t there? How many other nurses only counted for 15 seconds, leading to him not being bottle fed?
The previous day I was told he had a heart murmur. I questioned it, as it was the first I had heard anything about it. After looking at the records, they had been hearing it for almost a week, yet no one told me. My mom and I sat in on rounds the day after he was given someone else’s milk, and I found out IN ROUNDS that not only did he have a murmur, he had a hole in his heart. He was scheduled for an ultrasound of his heart that day, and had one several weeks ago, but I was always told that it looked good, everything came back normal. In reality, that was when they first saw the hole, but that entire time I had not been told. Not ok.
I had been thinking about transferring him to a different hospital almost from day one. I was thinking more and more about it once we started having issues. Eventually, I was thinking VERY seriously about it. I didn’t want to move him far away from me (Roanoke or Charlottesville), which is why I hadn’t done so before. But at that point I felt like I should have done it a week earlier and I should have seen the problems coming. I honestly thought that I was endangering my baby by leaving him in that NICU alone. I no longer trusted anyone there. I did not believe he was safe, or that they cared about him and his progress at all. The only thing holding me back was the cost. I would have to pay out of pocket to transfer him, and it would cost several thousand dollars.
Well, July 21st, two days after the wrong breast milk incident, I had just finished breastfeeding Levi and it was time for him to take his bottle feeding. What do you know, the bottle the nurse handed me had someone else’s name on it. (It is still so hard for me now to contain my anger as I write this. I don’t understand how a hospital could ever let this happen. Not only once, but twice. And KNOWING about the previous incident, you would think they would pay extra close attention.) My mom took a picture of the bottle and then we confronted the nurse. She insisted that it was my milk, she had just put the wrong label on it. She was totally expecting me to still give him the bottle, with someone else’s name. Maybe it WAS my milk, but if it wasn’t labeled correctly, how could she know that? And I’m pretty sure it would be against protocol to give a baby mislabeled milk, even if you KNEW it was the right milk. Even more upsetting, I have no doubt that if I had not been there, Levi would have been fed that milk.
 Mama Knows Best
Mama Knows Best
That was the last straw. Mama was mad. I went straight the unit manager and demanded Levi be transported. The manager said because it was not “medically necessary” the insurance wouldn’t cover it. I kindly reminded her of all the medical malpractice that had been going on in that unit, and that, to me, this was indeed medically necessary, because her staff was clearly inept. She claimed that she would “look into” the hospital absorbing the cost for transport. That was Thursday, July 22. Friday she came back and told me once again, it was not medically necessary. I felt helpless. I felt like the one thing my baby needed, I couldn’t seem to make happen.
From then on I called hourly. I questioned every single decision. I called not only the nurses, but the doctors as well. I argued with the doctor who wanted to put Levi on diuretics. Apparently I pissed her off, because an hour later she called me back and asked if I still wanted Levi to be transported. She apparently had gone to the unit manager and told her about our conversation, most likely how she was fed up with being questioned by a 22 year old, and the unit manager agreed to personally cover the cost!
And OH the difference! Levi THRIVED once we got to Roanoke, and I did as well. I finally felt able to step down as medical inspector and just be mom. I cried, this time not from stress and helplessness, but with relief and from happiness. Each incubator had a big comfy chair and curtains surrounding it - privacy! It was like a castle and VA Baptist had felt like a dungeon. I got to hold him as much as I wanted. He bottle fed every feeding - respirations were never an issue to them. They wanted to start breastfeeding as soon as possible, and get him out of the incubator as soon as possible. They could not believe he was still in one - he barely fit at this point.
The BEST difference was the doctors and nurses. Once the doctor heard (through the grapevine) that I didn’t  totally understand something, HE called ME immediately to make sure I understood everything. I have never experienced a doctor CALLING someone just to explain what may have been misunderstood. I really wasn’t even at the point of needing further explanation, but he wanted to make sure I was totally comfortable. Night and day. The difference was incredible.
totally understand something, HE called ME immediately to make sure I understood everything. I have never experienced a doctor CALLING someone just to explain what may have been misunderstood. I really wasn’t even at the point of needing further explanation, but he wanted to make sure I was totally comfortable. Night and day. The difference was incredible.
Also, in Lynchburg, I had to buy my own bags to store breast milk. At Roanoke, they had an endless supply of bottles. I swear I had previously spent over $100 on the bags, so this was super exciting to me. They also label and SCAN their milk, just as if it’s a medication. And they don’t just scan it once, they scan it TWICE. When they are mixing breast milk with the fortifier, they scan the milk as they put it in the mix. Then the mixture gets a new label, and they have to scan THAT before giving it to the babies.
I got to stay at the Ronald McDonald house, in walking (or biking) distance to the hospital (yes, I did bike there... often). It was so not what I was expecting - I thought it would be kinda dirty, I mean it’s free. But it was like a 5 star hotel - GORGEOUS! They served free dinner every night and had a stocked kitchen I could help myself to all day. There’s a library, formal living room, dining room, kids play room, TV room, laundry room (they even supplied detergent!).
The night my water broke, the lady from my church that met us at the hospital told me about another woman, Robin, from our church who was going into an emergency c-section at only 29 weeks. Her baby, Rhiley, was born at only 1lb 8 oz and was in the NICU at Roanoke, as well. We had never met before, but we were able to connect in Roanoke. It was so nice to have someone who understood exactly what I was going through without saying anything.
The second day in Roanoke a speech pathologist came to see us and help feed Levi, She analyzed how he sucked on his pacifier, then how he ate, a nd tried several different nipples on the bottle. She determined he should use a slow nipple and needed to be paced. He sucked way too fast and held his breath. So after he sucked a few times, I learned to pull the bottle away and make him breathe before he could have more. She also showed me what position he should eat in - the “elevated side lying” position. I didn’t even know speech pathologists did that kind of stuff. I also got to meet with a lactation consultant and Levi caught on right away.
nd tried several different nipples on the bottle. She determined he should use a slow nipple and needed to be paced. He sucked way too fast and held his breath. So after he sucked a few times, I learned to pull the bottle away and make him breathe before he could have more. She also showed me what position he should eat in - the “elevated side lying” position. I didn’t even know speech pathologists did that kind of stuff. I also got to meet with a lactation consultant and Levi caught on right away.
Levi progressed SO fast once we were in Roanoke. I say this a lot, and I don’t think this was really happening, but it was almost like he was being drugged at Lynchburg, and once we got to Roanoke he was alive again. He just kept surpassing every expectation and meeting every requirement needed to go home. And low and behold, July 31, less than a week after arriving in Roanoke, weighing in at 6 lbs 5 oz, I finally got to take my baby home!
--
Today Levi is a healthy 2 year old little boy, and no one would be able to guess what he went through as an infant. I sincerely hope that this story does not cause anyone anxiety, but rather encourages you to educate yourself and not be afraid to question the doctors. Doctors and nurses are overworked, have too many patients, and are subject to human error. You are the only person who is solely concerned with yourself or your baby, so don’t be afraid to stick up for yourself. If a doctor ever seems to have an issue with you asking questions, that’s when there’s a problem. Seek out a new doctor, find someone who will listen, and take the time to explain.
--
If you have a birth story you'd like to share with our readers, please submit it here.
The Motherhood Collective is on Facebook. Like us, then comment on our giveaway post for a chance to win a family photo shoot from Adam Barnes Photography. Our contest ends when we hit 500 Likes!