November is Prematurity Awareness Month. According to March of Dimes, there are 15 million babies born prematurely every year, with one million of those babies not surviving. We at The Motherhood Collective want to bring education and awareness to this issue, and to offer support to mothers and families. Here, we share a beautiful story of not only surviving, but thriving.
I had the perfect pregnancy. No morning sickness, no nausea, no fatigue, normal blood tests, normal blood pressure, no problems at all. Until I was 31 weeks. Our sweet daughter, Naomi Kathleen, was born at 9:11pm, on Sunday, November 8, 2009 weighing in at 2 pounds 7.9 ounces (the .9 ounces means a lot when you have a preemie) and measuring 14 inches long. Her due date was January 9. I was 31 weeks pregnant, meaning she was nine weeks early; however, the doctors said she had stopped growing around 28 weeks so she was especially tiny for her age.
I only remember bits and pieces and random images from the days after my daughter was born – images of my sweet husband crying ...images of an emergency code being called on the hospital intercom and more than 20 doctors flooding the room, shouting out symptoms and possible diagnoses …images of family members hugging and crying …images of being rushed to surgery …and a vivid image of being in the OR and a nurse on the IV team saying, “I need more time” as she stuck me over and over again trying to get the IV in my vein. I was so swollen that it made her task nearly impossible. One of the clearest memories from that time was that I didn’t even care what was going on. I knew she was poking me with no end in sight, but I honestly didn’t feel a thing. The pain in my chest was unbearable, and nothing else mattered. I finally just passed out from the pain, because I don’t remember anything more until a few days later – and those memories also remain fuzzy. The doctor later told me that when a person is facing that much trauma in such a short amount of time, their body goes into survival mode. Certain body parts literally shut down – and I’m sure that my brain began shutting down as my body fought to stay alive. I was later told a summary of what happened to me.
An hour before my daughter was born I was diagnosed with preeclampsia. They rushed me into the ER to complete an emergency c-section. The next morning, my blood pressure dropped so low that the doctors couldn't get a reading. I spent the next three days in the ICU, where it was determined that I had a rare disorder called HELLP syndrome. H stands for hemolysis, EL – elevated liver enzymes, and LP – low platelets. The most serious thing about my case of HELLP syndrome was the low platelets and the elevated liver enzymes. My liver began quickly shutting down, thus elevating the liver enzymes. At the same time, my platelets were at dangerously low levels. Platelets are what helps you clot – an essential element when your entire uterus has just been cut open. So because my uterus (a major organ during pregnancy) was not clotting, and I was internally bleeding to death.
They rushed me into surgery and performed a uterine artery embolization, which is where they permanently sear close the arteries leading to the uterus with the hope that if you stop the blood flow to the uterus, the uterus would stop bleeding out. While I was in surgery, they performed another surgery where they inserted an IVC filter into my Inferior Vena Cava (the main vein that brings all of the blood from your lower extremities to your heart, lungs, and brain). I had multiple blood clots in my lungs (Pulmonary Embolus) – something not normally associated with HELLP syndrome but an equally grave condition.
After surgery I went to the Intensive Care Unit, where I remained for the next three days. That was a very critical time for my recovery. Praise God I didn’t throw any more blood clots and the uterine embolization succeeded in stopping the internal bleeding. I had multiple blood transfusions and tubes inserted into my lungs, and with the help of some very strong medicine my liver slowly began functioning normally again. The trauma of the previous few days had literally taken every ounce of my strength, but I was now on the long road to recovery.
When my health and strength increased, I no longer needed to be in the ICU. The doctor released me to the telemetry (heart) unit where I spent the next 10 days. I was put on the telemetry floor because they felt as though my heart had suffered so much trauma that I needed to be on a heart monitor 24/7.
I wish I could describe the feelings I had as I left the ICU. I had no idea how bad it was there as I had stayed in my bed behind my curtain (mostly asleep/unconscious) the entire time. As they wheeled me away in the bed, I saw the other patients and they literally looked like death. They were all clinging to their lives – fighting for another chance to live. Had I been one of those people for the past few days? This was the first time the severity of the situation hit me. But I couldn’t dwell on that for too long. Before I was wheeled away to my new room, I would get to see my baby girl for the first time since her birth!
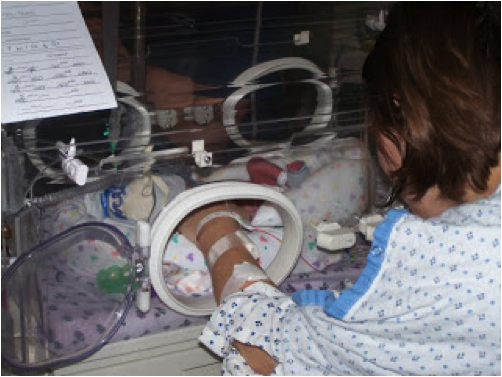
I cannot even begin to describe the feelings that overcame me the moment I saw her. She was still too small to be held, so I could only admire her by looking through her isolette. They allowed me to stick my hand through the holes, and I rubbed her soft skin. I couldn’t help but notice that she was a very muscular little girl, as she literally had not an ounce of fat on her body. Her whole body was perfectly defined. They assured me that she was doing great – just about ready to come off of CPAP (breathing devices) to see if her lungs would be able to hold their own pressure. This was basically an informative visit and I was caught up to speed on her condition - and this was now the best medicine for me. The doctor would only release me from the telemetry unit for one hour each day, under private nurse care. So for one hour a day, I would sneak off the the NICU to see my baby. That one hour each day was filled with moments of pure joy.
I was released from the hospital after two weeks, and I would come visit Noami each morning and evening. I will forever cherish the time we spent in the NICU. It was a beautiful time where we watched our child grow before our eyes and saw our prayers being answered daily. We received the best instruction for first time parents on how to feed our baby and how to diaper our baby, as well as the plethora of the additional information given to parents of preemies. A nurse once called Naomi a “feed and grow baby,” which she said was basically a baby you feed and just watch her grow. Toward the end of our NICU stay, that same nurse told us that she had been working in the NICU for over ten years, and she had never cared for a 2 ½ pound baby who never had a single setback …until now. Our Naomi was certainly a fighter.
We brought Naomi home 38 days after she was born. She now weighed 4 pounds 5 ounces. She continued to grow at home where I could now care for her 24 hours a day. I exclusively pumped for 10 ½ months, and stopped only when I had to travel to Standford University Hospital for a follow up surgery. (I was not going to lug my hospital grade pump through an airport on multiple connections!) Every day has been a gift since then. 19 months later, we welcomed home a baby brother through the amazing gift of adoption. I cannot have any more biological children, but looking back I am genuinely thankful for my experience - for the doctors and nurses who cared so diligently for us, for the many people who prayed, and for the Lord who answered those prayers. I am so thankful for this second chance at life, and for the privilege I have of being a momma to my two amazing and beautiful children.
For more information on preeclampsia and HELLP syndrome, please visit preeclampsia.org
Katelyn is a former high school English teacher turned stay at home mom. She loves her sweet husband, her dear friends, and her little life in Lynchburg.